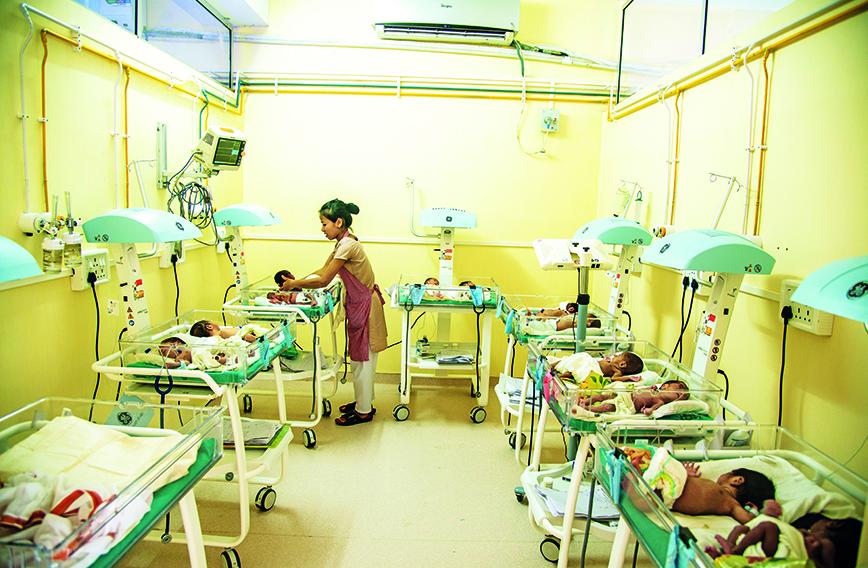
A neonatal care unit in a mission hospital
Low-cost mission hospitals hang in amid rapid change
Vijay Anand Ismavel
 THE first Protestant Christian mission hospital in India was started in 1870. Many of the early mission hospitals were established in remote rural areas or small towns and were focused on women and children or marginalized groups such as leprosy, tuberculosis and HIV patients. The first leprosy hospital was started in Purulia, West Bengal, in 1888 and continues to function today, run by The Leprosy Mission Trust India.
THE first Protestant Christian mission hospital in India was started in 1870. Many of the early mission hospitals were established in remote rural areas or small towns and were focused on women and children or marginalized groups such as leprosy, tuberculosis and HIV patients. The first leprosy hospital was started in Purulia, West Bengal, in 1888 and continues to function today, run by The Leprosy Mission Trust India.
The Medical Missionary Association, set up in 1905, later became the Christian Medical Association of India (CMAI) and continues to provide coordination to the Protestant Christian medical mission network in India. The Catholic Christian hospital network in the country is coordinated by the Catholic Health Association of India (CHAI), established in 1943. The first nursing and paramedical training institutions as well as many of the modern schools and colleges in the country were established by mission bodies.
After India gained independence, many expatriate staff returned to their home countries. In the 1970s and 1980s, the government required the remaining expatriate medical staff to leave. This led to a loss of support from their overseas supporters which in turn resulted in the closure of many mission hospitals at that time.
At present there are about 270 Protestant Christian hospitals and 600 Catholic Christian hospitals functioning in the country.
In the past 20 years, rapid changes have affected the way mission hospitals function, just as they have affected other ‘not for profit’ hospitals.
In the past, many of the mission hospitals, especially those in remote rural areas, were manned by a single long-term doctor or a small number of doctors who did everything — they could manage medicine, paediatrics, surgery and obstetrics. Some of the doctors could do orthopaedics and basic neurosurgery, paediatric surgery and provide other services.
At present, most young consultants are trained in a sharply focused area of medicine. The medicolegal and regulatory environment has also changed considerably, requiring consultants to stay within their area of expertise. This has ended the days of the intrepid, adventurous, highly trained consultant who could manage most medical/surgical cases confidently and replaced them with multi-departmental hospitals with consultants in each department.
CHARGING FEES
Many of the old mission hospitals could provide free or subsidized treatment to all who came to them because they were supported by donations, equipment and manpower from churches in the developed world. Such support has been severely curtailed by loss of interest from overseas donors and increased regulation of foreign donations by the government.
At present, mission hospitals generate most of their income from patients. In most hospitals patients in private wards pay more so that the patients in the general wards can be subsidized or given charity although there are mission hospitals, like the Makunda Christian Hospital in Assam, that have no private rooms and exist solely for the poor.
Indian entities, such as philanthropic foundations, churches, government grants and CSR-giving companies have replaced some of the external donors.
Insurance payouts from the government (Pradhan Mantri Jan Arogya Yojana (PMJAY) scheme), as well as various state government schemes have contributed to the income of these hospitals with many patients opting to avail of this cashless reimbursement facility. Maintaining financial sustainability and yet being poor-friendly has become a tight balancing act.
COMPETITION
When they were established, many of the mission hospitals were in very remote areas connected by poor roads. Slowly, entire towns with many other hospitals grew around them, leading to a lot of competition. Further, government hospitals provide free or highly subsidized treatment and corporate hospitals provide exclusivity at costs that a growing number of people can afford.
There have been several mission hospitals have not been able to adapt to the changing scenario and have therefore closed while some others were taken over by ‘for-profit’ entities. The remaining mission hospitals have evolved successful models to sustain themselves and thrive, continuing to provide healthcare to the poor and marginalized in spite of these challenges.
Mission hospitals were established with the motive of sacrificial service — most of them will have the words ‘for the poor and the marginalized’ and ‘in the spirit of Jesus Christ’ in their founding documents. Staff worked under many challenges which affected their personal and professional lives because of their commitment to Christian service. Many of them experienced heavy workloads, low salaries and many other inconveniences. Living conditions were less than ideal and children had to be sent off to distant schools.
It is not easy to recruit and retain people with such an altruistic worldview. India produces ever greater numbers of doctors each year, but this has not changed their distribution — they continue to be low in number in remote areas and in poor parts of the country. There is great disparity within and between Indian states — the multidimensional poverty index is 0.7 for Kerala and 50.9 for Bihar and this disparity is reflected in the number of doctors per capita as well.
NEW SERVICES
Many mission hospitals have repositioned themselves to adapt to the changing scenario around them. There are hospitals that provide geriatric care or palliative care, having moved from the traditional areas of obstetrics and surgery. Some have continued to compete with other hospitals by attracting patients with better quality of service in urban areas and by larger volumes of poor patients in rural areas.
India has seen a major movement towards commercialization of healthcare which is quite pronounced in the ‘for profit’ sector. Large hospitals acquire the latest equipment and attract top specialists by paying volume-based remuneration.
At the other end, government insurance schemes provide cashless reimbursement to poor patients but many of the procedures that were the mainstay of mission hospital income have now been reserved for government hospitals. This has led to hospitals constantly having to reposition themselves by finding patients and services that are falling through the gaps. They are thus God’s instruments of care in a world of need.
MEETING CHALLENGES
Despite these challenges, many Christian hospitals have grown from strength to strength. The Christian Medical College, Vellore, was started in 1900 and its hospital has expanded considerably in the past 20 years with a large new campus, housing 1,500 additional beds with tertiary/quaternary care facilities being inaugurated in 2022. Patients from all over the country and abroad come in increasing numbers to this institution, attracted by its ethical practices.
The larger mission hospitals offer medical, nursing and paramedical training programmes. Many of them offer the DNB course for postgraduate medical training as well as all levels of nursing and paramedical training affiliated to nursing councils (some through the Christian Medical Association of India which pioneered many of these programmes in the country).
RESURGENCE
There is a resurgence of interest in medical missions with many young Christian healthcare students belonging to Gen Z exploring the possibility of serving in needy parts of the country. They are willing to delay the gratification of getting into postgraduate courses as soon as possible and earning attractive salaries in the corporate world or abroad. The future of mission hospitals in the country rests on the shoulders of these young men and women.
New mission hospitals and services are constantly being started in many parts of the country. Many of the mission hospitals have received accreditations such as from the National Accreditation Board for Hospitals (NABH), National Neonatology Forum and others which testify to their high quality of services despite their relatively low costs of treatment.
Many mission institutions provided comprehensive care. The mission compound often had an English medium school and college as well as health and development projects in the surrounding villages. In the past 20 years, despite mushrooming of educational institutions across the country many old mission institutions continue to provide high quality training wherever they are located, having earned the trust of several generations. The Leprosy Mission Trust India is the largest provider of services to those affected by leprosy in the country today — their network of hospitals, vocational training centres and research centres continues to provide succour to this marginalized community. Other hospitals are focused on eye work, performing cataract surgeries to large numbers of people and curing them of their blindness.
With increasing numbers of patients affected by mental health issues and cancer, new opportunities to care have opened up. Some of the mission hospitals have also moved into super specialist services such as cardiology, neurosurgery, urology, and nephrology. During the recent Covid pandemic, mission hospitals were at the forefront of Covid care in the country.
What is the future going to be like? With the patient increasingly suspicious of the healthcare provider, hospitals which provide dependable care and are run with a spirit of service will remain in demand.
India continues to be a country with low investment of public funds in healthcare and a high rate of ‘out of pocket’ expenditure that drives large numbers of people to destitution from a single major healthcare event. Hospitals that can reinvent themselves and find ways to provide lifesaving treatment at affordable costs to those who fall through the gaps will make transformational impact in the India of tomorrow. Mission hospitals have mostly been invisible in the past and many of them will continue to be so in the future.
Dr Vijay Anand Ismavel ran the Makunda Hospital with his wife, Ann, for 30 years. He is currently at the Christian Medical College in Vellore.
Comments
-

Pierson David - Sept. 29, 2024, 12:04 a.m.
Thank you for highlighting the status of the mission hospitals. I have started a blog to www.megahealthindia.blog/missions to have a platform for like minded professionals to join hands.
-

Shobhana J. - Feb. 14, 2024, 12:42 p.m.
Such an inspiring read. The spirit of service is something our society can and should thrive on. This is truly such a beautiful sentiment and shows humane, kind and selfless acts are still very much in fashion. Hats of to the hardworking doctors in mission hospitals who work in such tough environments to serve those who need it most.
-

Sankar Daniel - Feb. 9, 2024, 7:57 p.m.
"Hospitals which provide dependable care and are run with a spirit of service will remain in demand." - True. People can compete with infrastructure, and other factors but the spirit of service will always be in demand.



