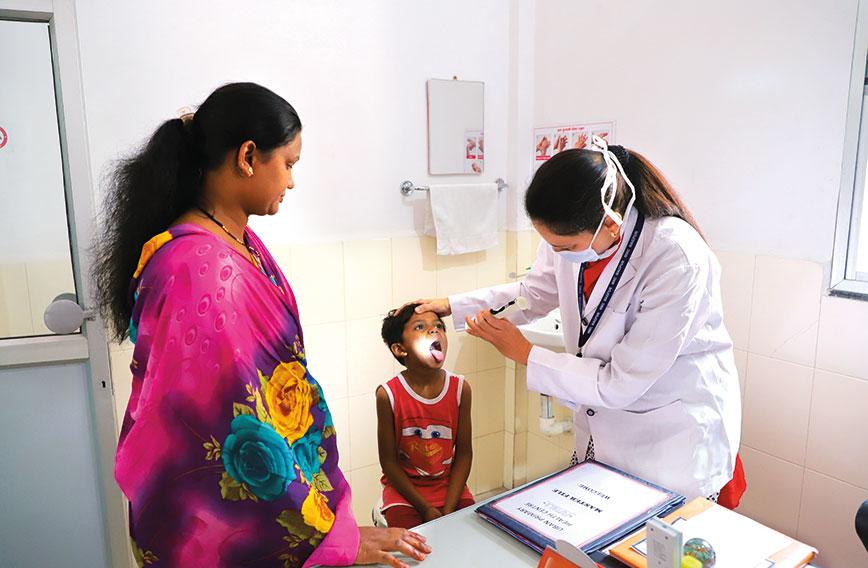
A primary health centre that has been upgraded in Nagpur| Photograph by Shrey Gupta
It is primary health care that people need
BY H.S.D. SRINIVAS
 India’s disease patterns have been shifting as cities grow and pull in more people. Lifestyle diseases like diabetes and hypertension have come to replace communicable diseases. There are more heart attacks and strokes and fewer people die from cholera and malaria. Also, there are fewer cases of mothers and babies dying during childbirth.
India’s disease patterns have been shifting as cities grow and pull in more people. Lifestyle diseases like diabetes and hypertension have come to replace communicable diseases. There are more heart attacks and strokes and fewer people die from cholera and malaria. Also, there are fewer cases of mothers and babies dying during childbirth.
Currently, urban areas are dominated by facilities in the private sector — clinics, hospitals and specialty centres. Pricing is unregulated. These private sector facilities have grown in the recent past and have come to be identified as the chief source of treatment.
The government sector, on the contrary, has witnessed neglect and decline. It has urban primary health centres (PHCs), maternity hospitals and hospitals attached to government medical colleges. It is an extensive system but its potential has not been fully exploited, particularly at the lower level like the PHC.
Like the rich, the poor use private facilities but much less than they should because of cost, access and availability factors. The result is they don’t tend to seek or avail of treatment at the appropriate time. They also overload the tertiary hospitals either at the time of emergencies or with complaints that should be dealt with at lower levels of the healthcare system.
What is needed is a healthcare system designed to tackle changes in the disease burden and the growing numbers in cities as urbanisation continues unabated.
The solution lies in a primary care network, both public and private, that includes OPD consultation, basic lab diagnosis, medicine dispensing and a workforce that can run targeted outreach programmes to enable access to basic health services for the marginalised population.
The urban PHC needs to serve as a hub to educate people on all aspects of communicable and non-communicable diseases. Another important function for the PHC is to act as a ‘gatekeeper’ by identifying people who need treatment and sending only those who need secondary and tertiary care to the bigger hospitals.
Governments may also like to use a primary care workforce for disease surveillance and epidemic control, convergence with disease control programmes run by national and state governments, data collection and record management for effective monitoring.
The last few years have seen many innovations tried out by the centre and the states. These include innovations in telemedicine to monitor and support primary care in towns and cities of Andhra Pradesh through outsourcing of out-patient services to private providers. Rapid response to life-threatening conditions like heart attacks in Tamil Nadu is being tried out nationally now. Mohalla Clinics in Delhi utilise the services of retired doctors for primary health issues and use health ATMs for supply of quality generic drugs. Basti Dawakhanas in Hyderabad are linked to free diagnostics in a hub-and-spoke model in Telangana.
The latest effort by the centre to upgrade more than 125,000 sub-centres in rural and urban areas by transforming them into health and wellness centres offering comprehensive primary care services, as being demonstrated in some parts of Kerala, if executed properly could ring in huge benefits by making appropriate care in an appropriate setting accessible and affordable.
The private sector, with its significant management skills and strengths, can play a key role in augmenting the work of public health authorities by addressing distortions in supply of services, influencing right health-seeking behaviour among patients by making the right care available at the right cost in the right setting.
Some of the initiatives that have attempted to reduce fragmentation of private providers in health and improve access to good quality affordable care for the urban poor include the pyramid model of care followed by single-specialty hospitals like the L.V. Prasad Eye Institute.
Reliance Foundation uses mobile medical units in its Mumbai outreach programme to deliver primary care under the supervision of its specialists in its main hospital in Mumbai. Quality of care in primary care clinics set up by Swasth Foundation in the underserved neighbourhoods of Mumbai are monitored through a link to a command centre while Health Spring clinics in Mumbai have innovative health financing options for chronic care patients, and the like.
As a philanthropic effort to strengthen urban primary care, the Tata Trusts have been working with the Nagpur city administration to upgrade the urban PHCs to increase utilisation and give a better patient and provider experience. Numerous other philanthropic efforts, notably by faith-based organisations like the Ramakrishna Mission Hospitals, have ensured that a semblance of affordable, if not free, first-level care is made available to the urban poor.
There is, however, no single solution that fits all conditions and achieves all stated goals. To reach the multiple objectives of a rich primary care offering we can look at an integrated primary care model that includes elements linking upgraded infrastructure, new technology that makes specialist advice affordable and timely and cost-efficient chronic care management by making appropriate drugs available at an appropriate price.
A motivated and trained workforce would be at the heart of such a model. It is important to monitor quality and have soft skills to manage crowds. Data-based decision-making is essential. A team approach is required so that there is decentralised planning. A careful study of tasks should distribute responsibilities so that nurses and doctors can concentrate on delivery of care and other staff members can do much more than they are currently allowed to.
A source of reduction in unnecessary expenditure would be empowering patients through behavioural change communication among patients (and providers) for timely and appropriate treatment, empowering the generally literate urban population to self-manage their own illnesses more effectively and avoid unnecessary complications.
Most primary care efforts ultimately cannot sustain as standalone systems and need a large payer like the government to sustain the quality and timeliness of service. The other model is for a larger secondary and tertiary hospital to support primary care efforts for its own quality offerings and decongestion of its main hospital. Getting the equation between cost efficiencies and effective treatment remains the ultimate challenge in developing a robust primary care system for the country. Until such an alignment is perfected we will continue to have sub-optimal or unaffordable care.
H.S.D. Srinivas is Head, Healthcare, Tata Trusts
Comments
Currently there are no Comments. Be first to write a comment!



